|
Definition of Dupuytren's Contracture:
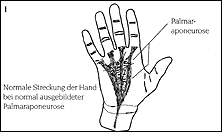
Dupuytren's contracture involves the scar-like, thread-shaped, taut shortening of the
so-called palmar aponeurosis. The palmar aponeurosis is a triangle-shaped plate of connective tissue located under
the skin of the palm. This type of tissue is also present in the rest of the body where it covers the musculature and
other structures with a considerably thinner 'skin' (fascia). This fascia (aponeurosis) is thickened like a plate in
the palm and on the foot sole even under normal conditions (Illustration 1).
The Dupuytren's contracture disease was first described in 1831 by Baron Guillaume Dupuytren, a famous French surgeon.
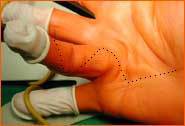
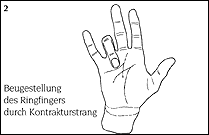
Due to nodule and cord formation between the palm and the finger, scar-like tension of the palmar aponeurosis can lead to
the contracture (bending) of one or more fingers (Illustration 2).
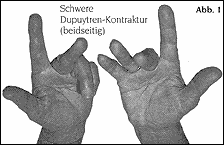
The severity of functional limitation depends more or less on the degree of contracture
(Figure 1).
Cause of Dupuytren's Contracture
The cause of Dupuytren's is unknown. It is likely that this disease arises along with other
diseases of the connective tissue. A relationship with liver disease, Diabetes mellitus and alcoholism has been discussed
but not proven. Genetic predisposition definitely exists as the disease often affects multiple family members. Dupuytren's
contracture affects men approximately eight times more often than women and usually manifests itself between the ages of 40
and 60.
Injury is not recognized as the cause of the onset of the disease and cases where the disease emerges after injury
are seen as coincidental. The hand sustains multiple minor and major injuries during our lifetimes, so that cases with a
causal relationship with Dupuytren's contracture must arise significantly more often.
Signs and Symptoms of Dupuytren's Contracture
The first sign is typically the formation of nodules in the palm of the hand, usually in the
area under the ring and little fingers and less often in the area of the other three fingers. However, the first sign can
also occur as nodules directly on the fingers in some cases.
Contracture of the skin in the area of the palm can also exist.
This occurs when the fibers that radiate out from palmar aponeurosis and into the fingers contract.
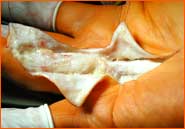
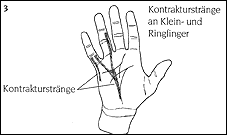
Dupuytren's cords
usually run lengthwise from the palm to the fingers, rarely diagonally, and sometimes reach over the entire finger.
(Illustration 3).
These cords cause the fingers to contract in towards the palm.
The advancement of Dupuytren's contracture can occur at various rates and sometimes comes to a complete standstill for longer periods of time.
However, degeneration of existing contracture is not to be expected.
Even when the contracture only affects one or two fingers, this can still lead to a severe limitation of the functionality of the hand.
Idiosyncrasies of Dupuytren's Contracture
- Normally the disease progresses slowly over a number of years with alternating periods of no change and disease advancement.
- In 15 - 20% of cases, contractures can also develop in the soles of the feet (Plantar fibromatosis), though these contractures
are as a rule not as pronounced as those of the hand and rarely require surgical treatment.
- The manifestation on both hands is sooner or later more or less assured, although the severity of the contracture on each hand can differ.
- The contracture usually first appears in the palm of the hand at the base of the little and ring fingers.
- Contracture occurs in the basal and proximal interphalangeal joint of the fingers.
- Flexor tendons are not involved in the contractures.
- The skin is often involved in the contractures.
- The Dupuytren's contracture is the nonmalignant growth of connective tissue.
- Dupuytren's contracture usually causes no pain.
- Reoccurence and new disease often occur.
Diagnosis of Dupuytren's Contracture
The typical clinical appearance secures the diagnosis. False diagnosis is almost impossible.
In rare cases, other tumors (epithelial cysts) can mimic Dupuytren nodules.
Treatment of Dupuytren's Contracture:
- Non-surgical:
- Clear success of therapy has not been proven with conservative treatment.
- Stretching exercises (both active and passive) can surely not hinder the progression of the disease, but may slow down contractions of the joints.
- Surgical:
The goal of surgery is to reestablish the functionality of the hand, rather than the complete removal of the contracture tissue.
Surgery is advised when the contracture of the affected fingers results in functional limitations of the fingers, causes pain or is perceived as a cosmetic encumbrance.
The occupation, hobbies and age of the patient play a significant role in the decision to perform surgery.
After the surgery, an intense physical and occupational therapy program is carried out for 3-4 weeks in order to achieve the desired functionality.
Anesthesia:
There are various possibilities for ensuring that the patient is free of pain during the surgery.
These possibilities will be explained to you by the anesthesiologist.
Technical Aspects of the Surgery
Surgery for Dupuytren's contracture is usually out-patient, that is, the patient can go home once the operation is completed.
1. General surgical preparation:
- Exsanguination:
In order to provide optimal viewing conditions and to reduce the risk of damage to healthy, neighboring
structures (nerves, vasculature, tendons) during hand surgery, so-called exsanguination is necessary.
The entire arm is wrapped in a rubber bandage which pushes the blood out of the arm. A cuff is then placed
on the arm to prevent blood from reentering the arm during the course of the surgery.
- Skin disinfection and sterile conditions:
In order to decrease the risk of infection, the skin is disinfected and the surgical field is covered with sterile cloth.
- Magnifying glasses:
The surgeon utilizes magnifying glasses in order to see and manipulate the hand structures as well as possible.
2. Sequence of surgical events:
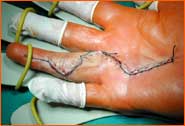
- Sketching of the incision (Illustration 4)
- Skin incision
- Careful dissection of the skin as thick as possible, in order to maintain blood circulation and prevent necrosis (death of tissue)
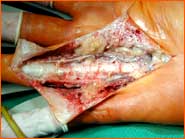
- Detachment of the cords and nodules of the modified palmar aponeurosis in the wrist area.
- Disconnection of the palmar aponeurosis from proximal to distal with consequent exposure of the nerve and vessel bundles that lead to the fingers.
- The dissection of the nerve and vessel bundles is typically more difficult in the area of the fingers. Even though the nerves do not adhere to the
contraction cords in first time surgeries they can wind around the cord in a corkscrew fashion.
- Contractures, usually of the middle joint, can typically be passively detached after the release of the cords. Depending on the severity of the
contracture, surgical release of the joint may also be necessary.
- After removal of the contracture tissue, the integrity of the nerve and vessel bundles is double-checked.
- The success of the surgery can be verified through sight and touch.
- Insertion of redon drainage to drain the blood after surgery in order to prevent a blood clot within the palm of the hand.
- Opening of the arterial tourniquet. Hemostasis initiated with the compression of the wound and then through electrocoagulation (heating) of vessels that are still bleeding.
- Closing of wound autverschluss
- Steel wool compression band
- Immobilization with splint
Post-operative treatment:
- The patient is allowed to return home after the surgery. The joints not in a cast should be moved but not heavily used.
- One day after surgery:
Cast and soft tissue control, and when appropriate the removal of redon drainage (although sometimes not until 2-3 days after surgery).
- Five to seven days after the surgery:
Removal of cast splint and bandage change, initiation of physical and occupational therapy (daily!).
- Fourteen days after surgery:
Bandage change and removal of stitches.
- The bandage is no longer necessary the day after the stitches are removed. Begin of regular (3-4 times daily) exercises in cold water
(with addition of ice cubes). Cold reduces swelling and pain. Patients that cannot tolerate cold should use lukewarm water.
- The scar treatment can begin five days after the removal of stitches.
The scar should be massaged with a fatty cream or salve 4-5 times daily so that the scar becomes softer, less painful, and more resistant
to stress ("toughening" of the scar). Also beneficial is the tapping of the scar, for example with a soft brush.
- The duration of the patient's incapacity to work is usually around 4-6 weeks.
Healing progression after the surgery:
Even after returning to work and the completion of physical and occupational therapy,
the patient must continue learned exercises for weeks or months in order to prevent scar-related contracture.
The prescribed flexor splint should continue to be worn for several more weeks until no change in the scar area is noticed.
Scar discomfort largely disappears after the first 6-8 weeks. After 3-6 months patients no longer complain of pain.
However, the scars final state is not reached until approximately 12 months after surgery.
© Dr. Klaus Lowka
 back to top back to top
|
 |
 |